Understanding the “Cicada” COVID-19 Variant: What You Need to Know
A New Variant Catches Global Attention
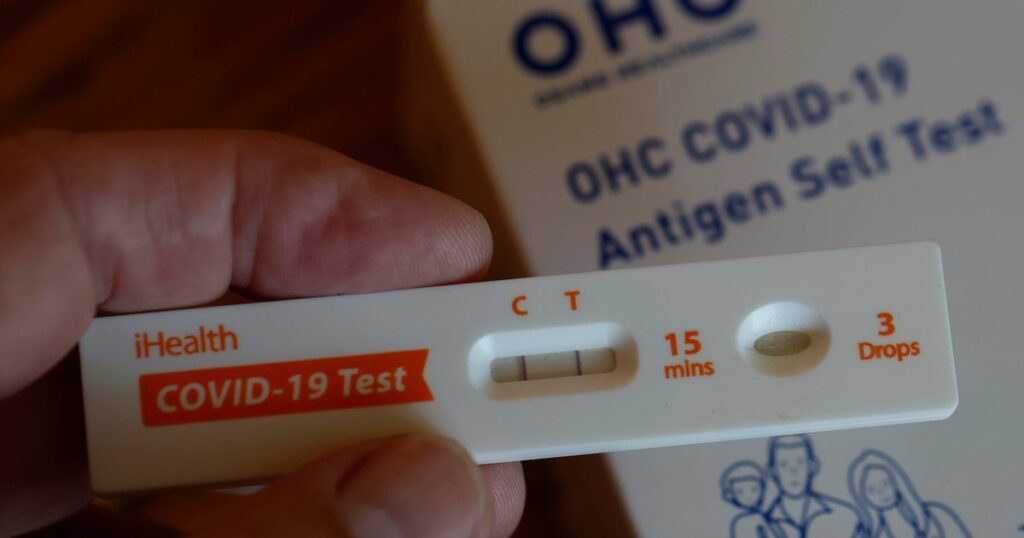
The term “Cicada” has been making headlines recently, but this time it has nothing to do with the familiar buzzing insects that emerge periodically in nature. Instead, health officials are using this nickname to describe BA.3.2, a new COVID-19 variant that has caught the attention of both the Centers for Disease Control and Prevention (CDC) and the World Health Organization (WHO). First identified in November 2024, this variant has been spreading across the globe, reaching at least 23 countries and making its presence known in 25 states across the United States as of February. While the variant is certainly spreading within American borders, health experts emphasize that it hasn’t become the dominant strain yet. Dr. William Schaffner, a respected professor of infectious diseases at Vanderbilt University, explained the situation with measured caution when speaking to CBS News, noting that “whether it will push itself to the front of the line remains to be seen.” This wait-and-see approach reflects the cautious optimism of health professionals who have learned from previous variants that predicting the exact trajectory of COVID-19 mutations requires careful observation and time.
The Science Behind This Highly Mutated Variant
The Cicada variant belongs to the Omicron family, which has been responsible for numerous COVID-19 cases over the past few years. What makes BA.3.2 particularly noteworthy from a scientific perspective is its high degree of mutation – researchers have identified between 70 and 75 mutations in this variant. This extensive genetic change has raised questions about how well our existing immune defenses can protect us. A recent study published in the prestigious medical journal Lancet shed some light on this concern, finding that the current COVID-19 vaccine shows reduced effectiveness against BA.3.2 when compared to the strains currently circulating most widely. However, the study also provided reassuring news: the vaccine does still offer some level of protection against this new variant. Dr. Schaffner acknowledged the preliminary nature of our understanding, explaining that “these are still early days,” but added that current evidence suggests “there is this capacity for this new variant to evade some of the protections we have all acquired over the years.” This ability to partially bypass our immune defenses, whether from vaccination or previous infection, is what makes BA.3.2 a variant worth monitoring closely, even if it doesn’t necessarily mean we’re facing a crisis.
Severity and Current Impact on Healthcare Systems
One of the most pressing questions about any new COVID-19 variant is whether it causes more severe illness than previous strains. Fortunately, the current data provides some reassuring answers. The CDC is not reporting any nationwide surge in severe COVID-19 disease at this time. In fact, the overall trends are moving in a positive direction, with case rates, emergency room visits, and hospitalizations all declining across the country. However, health experts caution that this national picture doesn’t tell the whole story, as individual states can experience very different patterns. For instance, Massachusetts and Florida are both estimated to be experiencing likely increases in COVID-19 cases, even as the national trend moves downward. Dr. Celine Gounder, CBS News medical contributor and editor-at-large for public health at KFF Health News, offered additional reassurance about the variant’s severity, stating that “we haven’t seen evidence of this variant causing more severe disease or an increase in hospitalizations elsewhere.” This information suggests that while BA.3.2 may be spreading and may have some ability to evade immunity, it doesn’t appear to be causing more serious illness than other circulating variants. This is crucial information for both public health officials and the general public as we continue to navigate life with COVID-19 as an ongoing presence rather than an acute emergency.
Recognizing Symptoms and Who Needs to Take Action
Despite the emergence of new variants, the symptoms of COVID-19 have remained fairly consistent throughout the pandemic, and BA.3.2 appears to be no exception. People infected with COVID-19 typically experience a familiar set of symptoms including fever, cough, shortness of breath, sore throat, and congestion. These symptoms can range from mild to severe and may appear anywhere from two to fourteen days after exposure to the virus. The CDC continues to emphasize the importance of vaccination, particularly for certain vulnerable groups. Specifically, the agency recommends that people ages 65 and older should get the current COVID vaccine, along with those who have never received any COVID vaccination. Additionally, anyone at high risk for severe illness from COVID should prioritize getting vaccinated. This high-risk category includes people younger than 65 who have chronic medical conditions such as heart disease, lung disease, or diabetes, as well as those who are immunocompromised due to conditions or treatments that weaken the immune system. For these vulnerable populations, even variants that don’t cause more severe disease in the general population can pose significant risks, making vaccination an important protective measure.
Timing Your Vaccine for Maximum Protection
Dr. Schaffner provided specific guidance about the optimal timing for COVID-19 vaccination, particularly with an eye toward patterns that have emerged over the past few years. He advised people to consider “getting a dose of the vaccine towards the end of May, beginning of June in order to provide some protection against the summer increase.” This recommendation is based on observed patterns from previous years, as he explained: “We anticipate that will happen because that’s what’s happened in the past.” This seasonal pattern of COVID-19 increases during summer months has become a predictable feature of the virus’s behavior, likely driven by a combination of factors including increased indoor gatherings in air-conditioned spaces, travel, and the natural waning of vaccine protection over time. By timing vaccination strategically before this anticipated summer surge, people can ensure their immune protection is at its peak when they’re most likely to encounter the virus. This approach represents a shift in how we think about COVID-19 vaccination – moving from emergency response to a more routine, strategic approach similar to how we handle annual flu shots, with timing based on expected periods of increased circulation.
Living with COVID’s Evolution
The emergence of the Cicada variant serves as a reminder that COVID-19 continues to evolve, and our approach to managing it must evolve as well. We’re no longer in the acute crisis phase of the pandemic, but neither has the virus disappeared. Instead, we’re learning to live with COVID-19 as an ongoing presence, much like we do with influenza and other respiratory viruses. The good news is that we have tools to manage this reality: vaccines that provide protection even if not perfect, treatments for those who do become seriously ill, and growing understanding of how the virus behaves seasonally. The monitoring of variants like BA.3.2 by organizations like the CDC and WHO represents an early warning system that helps us stay ahead of potential threats. While this variant has some concerning characteristics, particularly its high number of mutations and ability to partially evade immunity, it hasn’t translated into a surge of severe illness or overwhelmed hospitals. This outcome reflects both the virus’s evolution toward forms that may be more transmissible but less severe, and our own improved immunity through vaccination and previous infection. As we move forward, staying informed about new variants, maintaining up-to-date vaccinations especially for vulnerable populations, and following basic public health practices during periods of high transmission will remain our best strategies for keeping ourselves and our communities healthy.