The Reality of Weight Regain After Stopping GLP-1 Medications: What New Research Reveals
Understanding the Long-Term Effects of Popular Weight Loss Drugs
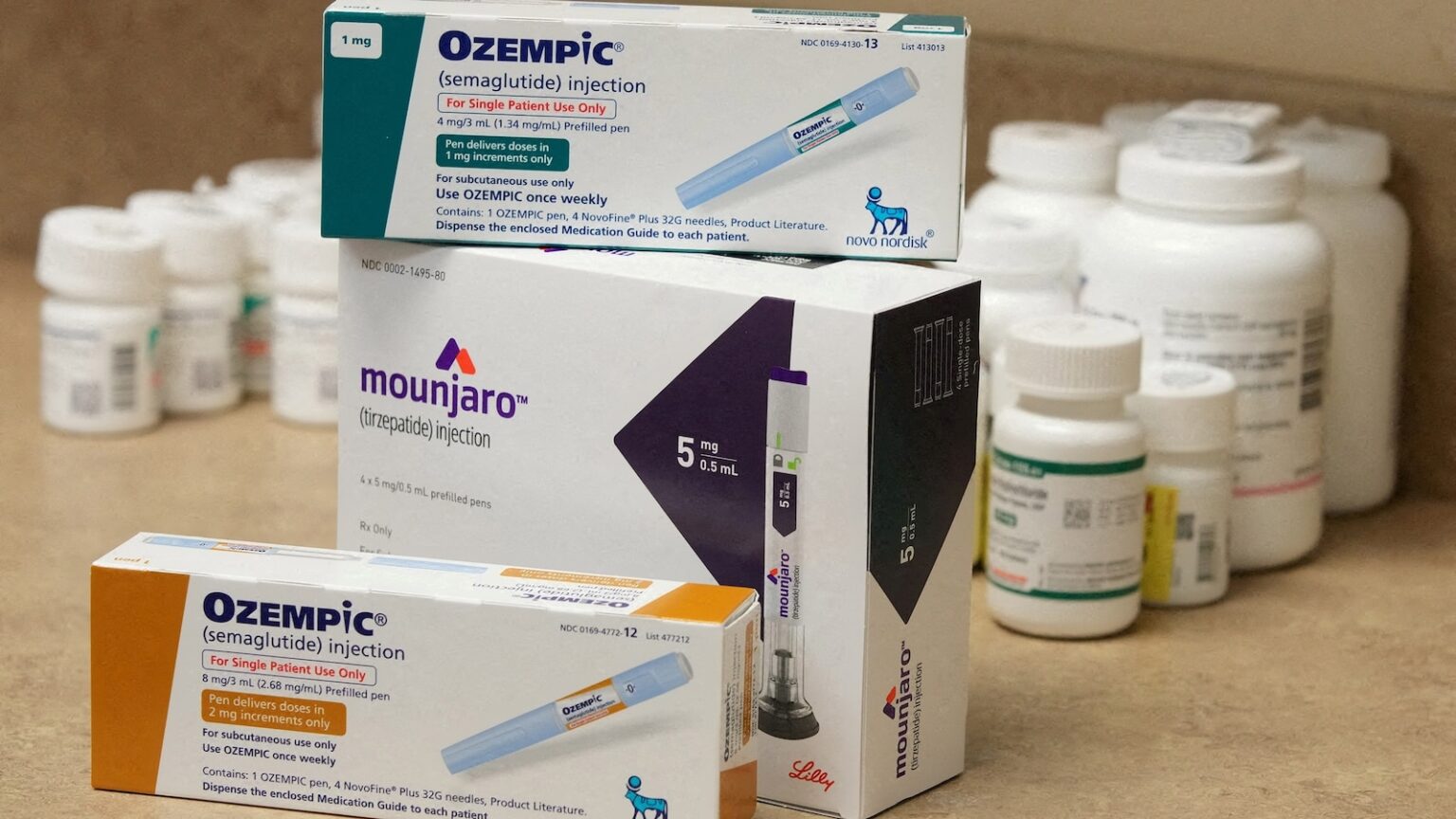
In the rapidly evolving world of weight loss medications, drugs like Ozempic, Wegovy, and Mounjaro have become household names, offering hope to millions struggling with obesity and diabetes. However, a comprehensive new study published in the medical journal eClinicalMedicine is shedding important light on what happens when people stop taking these medications—and the findings reveal a challenging reality that anyone considering or currently using these treatments should understand.
The research, released on Wednesday, represents one of the most extensive examinations to date of the long-term outcomes for people who discontinue GLP-1 receptor agonist medications. By systematically reviewing 48 different studies, researchers painted a detailed picture of what happens in the months and years after patients stop their medication regimen. The study examined outcomes for people using popular GLP-1 drugs including liraglutide (marketed as Victoza and Saxenda), semaglutide (sold as Ozempic, Wegovy, and Rybelsus), and tirzepatide (available as Mounjaro and Zepbound). What they discovered challenges the notion that these medications offer a permanent solution to weight management and instead suggests that for many people, these drugs may need to be a long-term or even lifelong commitment.
The Numbers Behind Weight Regain: What Happens When You Stop
Perhaps the most striking finding from this comprehensive review centers on how much weight people typically regain after discontinuing their GLP-1 medications. According to the analysis, patients who stopped taking these weight-loss drugs regained approximately 60% of the weight they had lost within just one year of stopping treatment. This represents a significant reversal of the progress many patients worked hard to achieve while on the medication.
Even more concerning is what the researchers discovered when they looked beyond that first year. Using sophisticated computer statistical modeling techniques, the research team projected what might happen to patients who remain off the medications for longer periods. Their models suggested that those who stay off the drugs could eventually regain about 75% of their previously lost weight. This means that if someone lost 40 pounds while taking a GLP-1 medication, they might expect to regain approximately 30 pounds if they discontinue treatment and don’t implement other weight management strategies.
These findings underscore a fundamental truth about obesity that medical professionals have long understood: it’s a chronic condition that often requires ongoing management, much like diabetes or high blood pressure. The body’s natural regulatory systems seem to push back against weight loss, working to restore the previous weight setpoint through increased hunger signals and decreased metabolism. When the medication that was helping to override these signals is removed, the body’s natural tendencies often reassert themselves, leading to the weight regain that the study documented.
Taking an Individualized Approach to Weight Management
Dr. Tara Narula, ABC News chief medical correspondent, appeared on “Good Morning America” to discuss these findings and emphasized that the research highlights the importance of personalized medicine when it comes to weight loss. Her insights reveal that there’s no one-size-fits-all approach to using these medications, and different people will have vastly different experiences when it comes to maintaining their weight loss after discontinuation.
“There are some people who can come off of them and maintain the weight loss,” Dr. Narula explained, offering hope that discontinuation doesn’t automatically mean complete weight regain for everyone. “There are others who will need to be on some sort of dose taper or some who need to stay on the same dose forever.” This perspective reframes how we should think about these medications—not necessarily as short-term interventions, but potentially as long-term treatments that may require indefinite continuation for optimal results.
The variation in individual responses likely stems from multiple factors, including genetic differences, metabolic variations, lifestyle habits developed during treatment, and the specific health conditions that prompted the prescription in the first place. Some patients may successfully use their time on medication to establish healthier eating patterns and exercise routines that they can maintain independently. Others may have underlying metabolic or hormonal factors that make long-term medication necessary for sustained weight management. Understanding which category you fall into requires close collaboration with healthcare providers and honest self-assessment of your ability to maintain lifestyle changes without pharmaceutical support.
The Study’s Limitations and What They Mean for Patients
While this systematic review represents one of the most comprehensive looks at post-treatment outcomes for GLP-1 medications, it’s important to understand its limitations. The research analyzed a remarkably diverse group of patients across the 48 studies examined, including people with various health conditions such as diabetes and kidney disease, individuals with different starting weights and target endpoints, and patients taking different medications within the GLP-1 class.
This diversity, while making the study broadly applicable, also means the findings represent averages across widely varying circumstances. Someone who took semaglutide for six months while following an intensive lifestyle modification program might have very different outcomes than someone who took tirzepatide for two years while making minimal behavioral changes. Similarly, a person with type 2 diabetes may experience different weight regain patterns compared to someone without diabetes who took the medication solely for weight loss.
These limitations don’t invalidate the research findings, but they do suggest that individual outcomes may vary considerably from the averages reported. This reinforces Dr. Narula’s point about the need for individualized treatment approaches. Your specific circumstances—including which medication you take, how long you take it, what lifestyle changes you make alongside the medication, and your underlying health conditions—will all influence what happens when you stop treatment.
The Silver Lining: Permanent Benefits May Be Possible
Despite the concerning statistics about weight regain, the research also revealed genuinely positive findings that offer hope for people using these medications. Dr. Narula pointed out that while patients regained a significant portion of their lost weight, they didn’t regain all of it. On average, people maintained a loss of about 4% to 5% of their baseline body weight even after discontinuing the medication.
“That’s not clinically insignificant,” Dr. Narula emphasized, highlighting that even modest sustained weight loss can produce meaningful health benefits. A 4-5% reduction in body weight has been associated with improvements in blood pressure, cholesterol levels, blood sugar control, and reduced risk of developing conditions like type 2 diabetes in at-risk individuals. For someone weighing 200 pounds, maintaining a 10-pound weight loss represents real progress toward better health outcomes.
Furthermore, there’s emerging evidence suggesting that time spent on GLP-1 medications might create lasting changes beyond simple weight loss. Dr. Narula noted that researchers believe some patients may be fundamentally changing their relationship with food and eating behaviors during treatment. “We think that some of these people may be changing behavior, nutrition, lifestyle, [and] also may be changing the hormones in their body by being on [GLP-1 medications], changing how their brain sort of operates or functions permanently,” she explained. This suggests the possibility that these medications might help “reset” some of the metabolic and neurological factors that contribute to obesity, potentially making it easier to maintain healthier weights even after discontinuation. Additionally, research indicates that dose tapering strategies—gradually reducing medication amounts over time rather than stopping abruptly—might help prevent weight regain by giving the body time to adjust to functioning without the drug’s support.
A Comprehensive Approach to Lasting Weight Management
The key takeaway from this research isn’t that GLP-1 medications don’t work or that people shouldn’t use them. Rather, it’s that these medications work best when integrated into a comprehensive, long-term weight management strategy rather than viewed as a quick fix or temporary solution. Dr. Narula emphasized that alongside GLP-1 medications, other proven strategies including lifestyle counseling, regular physical activity, and sometimes other medications can all contribute to successful long-term weight management.
For people currently taking or considering GLP-1 medications, this research suggests several important considerations. First, have realistic expectations about what happens if and when you stop the medication. Second, work with your healthcare provider to develop a comprehensive plan that includes not just the medication but also sustainable dietary changes, regular exercise, behavioral modifications, and ongoing support. Third, recognize that you may need to continue the medication long-term, either at your current dose or at a reduced maintenance dose, to sustain your results. Fourth, if discontinuation is planned, consider a gradual tapering approach rather than stopping abruptly. Finally, understand that even if some weight returns after stopping, maintaining even a portion of your weight loss delivers genuine health benefits that make the treatment worthwhile. The emergence of GLP-1 medications represents a genuine breakthrough in obesity treatment, but like most medical interventions for chronic conditions, they work best with continued use and as part of a holistic approach to health.